If you or someone you know has a disability and is struggling to pass exams, please see the main article, Managing Disability and Actuarial Exams in the Future Fellows Newsletter.
My Experience with Vestibular Migraine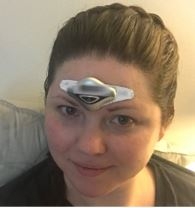
It started with mild motion sickness, just feeling a little bit queasy after taking the bus into the city. For the first almost 30 years of my life, I loved motion! As a kid, I selfishly monopolized the tire swing every time I went to the local playground. As a teenager, I spent every summer eagerly anticipating the Nez Perce County Fair, when I could ride the Zipper for three days straight. When I passed my first actuarial exam, I spent the next day at Silverwood on the Corkscrew and the Aftershock. When I moved to New York City, I fell in love with the subway: I could read or study on the train, how efficient!
But then the motion sickness started. First the bus, then planes and cars, and finally my beloved subway. I couldn’t read or study on the train anymore. I could barely make it to work without vomiting in a trashcan on the platform. Sometimes I would get mild headaches after work that could last for several days. It took three doctors, including a balance specialist and a neurologist, to diagnose me with vestibular migraine.
As the motion sickness escalated, the headaches increased in frequency and severity, and I started to notice additional symptoms. Many attacks now come with stabbing pain in my left temple. Some include intense visual or audio distortions; the room seems to be spinning, or I can’t understand spoken words. I may stumble around my apartment or have trouble getting warm. “Brain fog” makes it difficult for me to speak, either because I can’t find the words or my speech is slurred.
And it’s not just travel. Pressure changes due to oncoming storms, Intense smells, dissonant sounds, and high contrast images can all trigger attacks. I avoid action movies and television shows with flashing lights. Travel is still the biggest problem, though. If I have a month with fewer doctor visits, I might be able to leave my neighborhood for a special event, but I mostly try to get friends and family to come to me.
Fortunately, with the help of my neurologist and some personal research, I have also discovered improved prevention and acute treatments for attacks. A lot of things did not work: acupuncture, daith piercing, CBD oil,and a long list of prescription medications had little to no effect. However, after several years of trial and error, things seem to be improving thanks to dietary changes, meditation, a nifty little electrode device from Belgium (pictured), and several prescription medications, including a monthly injection of a CGRP blocker.
Are Exam Accommodations Fair?
When I was teaching high school math 10 years ago, I had students with a wide variety of disabilities, many which required accommodations. In an academic setting, this could be a support that allows a student to access knowledge. For example, let’s use an imaginary student named Kevin. Kevin has dyslexia, so the school provides him an audio version of the textbook. This type of accommodation is usually well accepted.
However, when it comes time for a student to demonstrate knowledge, especially via an exam, the accommodations are often more controversial. Some people will complain when Kevin takes a verbal exam or has an extended testing period to account for the extra time it will take him to read the questions.
I have never understood this disconnect; if we agree that Kevin needs an accommodation to access learning, why is it suddenly “unfair” to accommodate his ability to demonstrate learning?
So why did it take me so long to request to take my exams at home? I knew traveling to the exam site and sitting under fluorescent lights for five hours was increasing the difficulty of the exam experience and decreasing my ability to demonstrate my knowledge, yet I hesitated to check the box for accommodations on the registration form.
“I Have a Disability”
Every time I registered for Exam 6, I would see the box for accommodations and tell myself I couldn’t check it because “I don’t have a disability.” When I read what I wrote in the first section of this post, it seems like it should have been obvious, but acknowledging that I DO have a disability was surprisingly difficult. There were three key factors that made this such a challenge:
“You don’t look sick.”
Migraine is an invisible disease. Sometimes I get a little puffy around the eyes during an attack, but otherwise you would not know by looking at me that something was wrong. Even MRIs of my brain revealed nothing sinister. The lack of observable symptoms has led some to speculate that migraine patients are making things up or exaggerating symptoms for attention.
It is only recently that scientific studies have shown that migraine patients often have elevated levels of calcitonin gene-related peptides (CGRPs). While CGRP levels are not definitive and therefore not used as a diagnostic tool, this discovery did generate a race to market of several medications that inhibit CGRP reception in 2018.
Because of the success of CGRP-inhibiting drugs, understanding and attitudes about migraine are improving. However, migraine affects significantly more women than men. While feminism has made great strides in the last century, many women still encounter unexpected barriers when seeking healthcare, especially for female-associated diseases. This experience is magnified in society at large; it was only last year that I was told my train-induced nausea was “all in your mind.”
It doesn’t help that frequency, severity, and triggers of migraine symptoms can vary wildly from patient to patient, or even from attack to attack. I can’t tell you how many times an acquaintance has told me that they have migraines, but they just take an over-the-counter pain killer and a nap; why can’t I just get over it? On the other hand, I’ve also been told that it’s not a real migraine if I don’t end up in the emergency room (false!), which leads me to the next factor:
“It could be worse.”
I have a lot to be thankful for. I have a loving family and a great job. My health is not ideal, but a lot of people have things a lot worse.
As an “Elder” Millennial, I suspect a lot of Americans my age grew up with the idea that we shouldn’t complain because our lives were easier than that of our grand-parents: “At least it’s not the Great Depression!” Or that children in other countries were starving: “At least you have food on your plate!”
While a positive outlook is generally a good thing, this strange refusal to acknowledge anything negative has led to some interesting interactions with people my age and older. I believe most of these people are well-meaning when I explain my condition and they say, “At least it’s not cancer!” Well, yeah. At least it’s not a coma! At least I’m not DEAD! But here’s the crucial thing:
The suffering of others does not invalidate my own struggles.
I have to remind myself of this a lot. “Somebody else has it worse” is not a reason to ignore your own problems. You deserve to be as healthy as you can be!
“…back to normal.”
There is no known cure for migraine, but as my symptoms escalated, I kept thinking that with the right treatment regimen, I could still get “back to normal.” It has only been in the last year that I realized “normal” was not an achievable goal for my situation.
While it took me years to accept that things were never going to be the same, the hardest thing is that some of my friends and family are still not there. Some seem to think I haven’t done enough: maybe if I exercise 8 hours a day, stick to an all-fat diet, and sleep on a bed of unicorn hair, I wouldn’t need all these medications! Others accuse me of doing too much, suggesting I should avoid all possible triggers and basically just live my life in a light-proof, sound-proof bubble.
Obviously there’s a balance, which is why I try to focus on “living my best life with migraine.” I will continue to seek out medical intervention and self-care techniques that will help me manage the condition. And I will do my best to avoid triggers without completely disconnecting from the things that make life worth living. For example, while I avoid most unnecessary travel, I promised myself a trip to Paris once I achieved the ACAS credential, and I’m not giving that up, even if it means tacking on a few extra days to recover from the flight. On a smaller scale, the free time I used to spend on video games is now spent preparing to run my regular Dungeons & Dragons campaign.
I had to adjust my work and study habits, too. I mostly work from home, and I had to change the main way I memorize information before an exam. Details appear in the main article (link at top).
Figuring out what will work for you takes time, and it is helpful to have support from friends and family, a personal therapist, or a dedicated support group for your condition. Just know that even if your life isn’t turning out the way you planned, you can still find joy in a modified path.
Your Story
One of the biggest hurdles to inclusion is visibility. If you would like to share your story with disability, please log in and tell us about it in the comments below.